Understand and Manage Your Medical Benefits
Serving our communities and members with excellent and compassionate care. Through teamwork and innovation, faith and compassion, advocacy and action, we endeavor every day to keep you happy, healthy, and whole.
Select Plans
For specific CommonSpirit Health medical plan benefit information, provider networks, pharmacy benefits and more visit your plan specific page below.
About BRMS
Benefit & Risk Management Services (BRMS) has been selected to provide administrative services to your CommonSpirit Health benefit plans. We are dedicated to providing the highest quality service in claims administration and management of employer sponsored benefit plans.
BRMS can help you with ID cards, claims information, Explanation of Benefits statements, transition of care and much more!

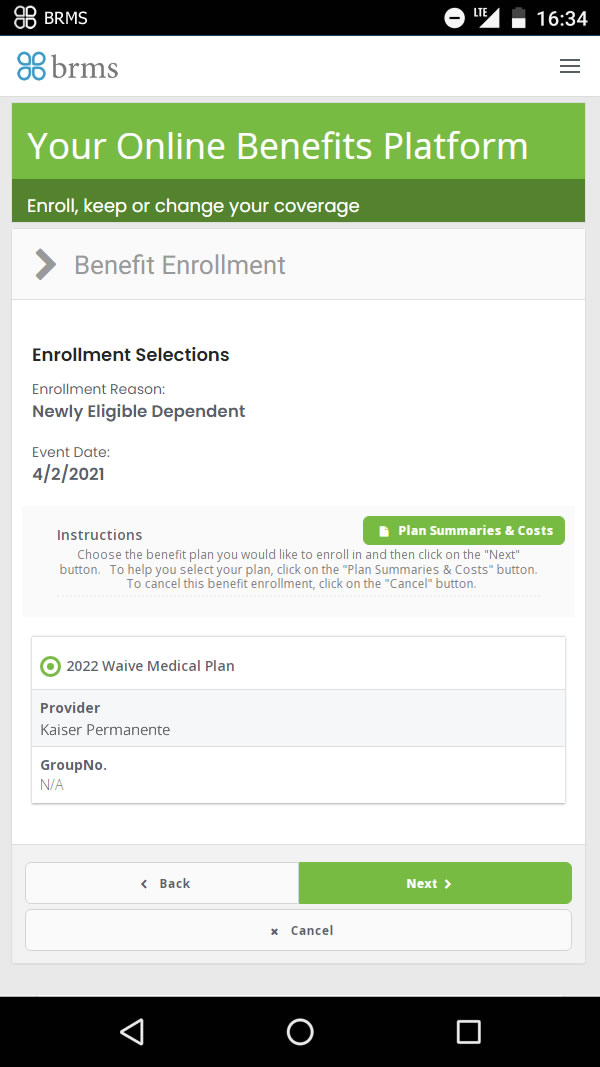
MyHealthBenefits.com
MyHealthBenefits.com is BRMS's online benefits resource designed to assist you in understanding and getting the most out of your benefit plan. As a member you can register on MyHealthBenefits.com.
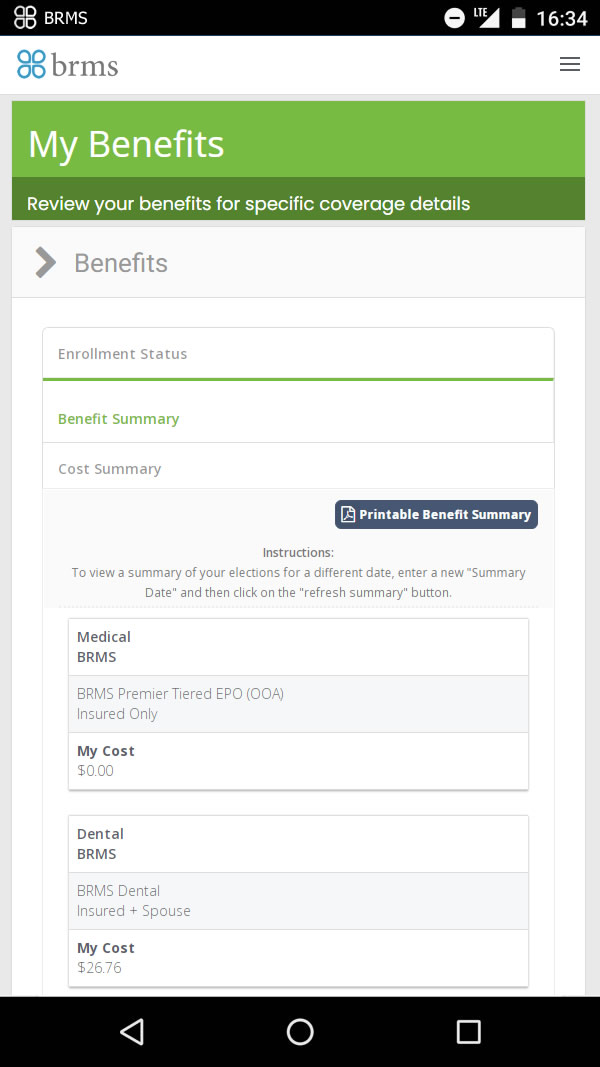
- View covered services under your benefit plan
- Track and manage dollars accumulated year-to-date toward your deductible and out-of-pocket limits
- View & print a copy of your ID card
- View and print explanation of benefits (EOB) statements
- Print claim forms
How Can We Help You?
For specific questions about the Dignity Health plan benefits or when you should be receiving your ID card please contact BRMS.
BRMS Customer Service:
Hours: Mon-Fri 7am-6pm PT
Central Coast Plans Call: 866-755-6974
Ventura EPOs & PPO call: 866-750-0576
For questions about your CommonSpirit Health benefits, call the CommonSpirit Health Benefits Contact Center.
CommonSpirit Health Benefits Contact Center:
855-475-4747, Press option 1
Hours: Mon-Fri 6am-5pm PT
Contact BRMS for help with Your Benefit Plan info:
You will receive a response within 24 hours for all inquiries submitted Monday through Friday. Inquiries submitted on Saturdays and Sundays will be responded to on the next business day.

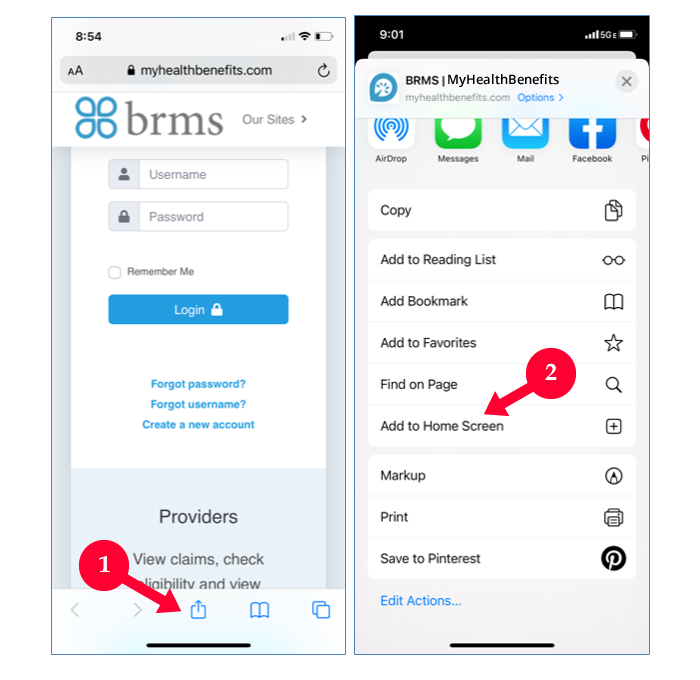
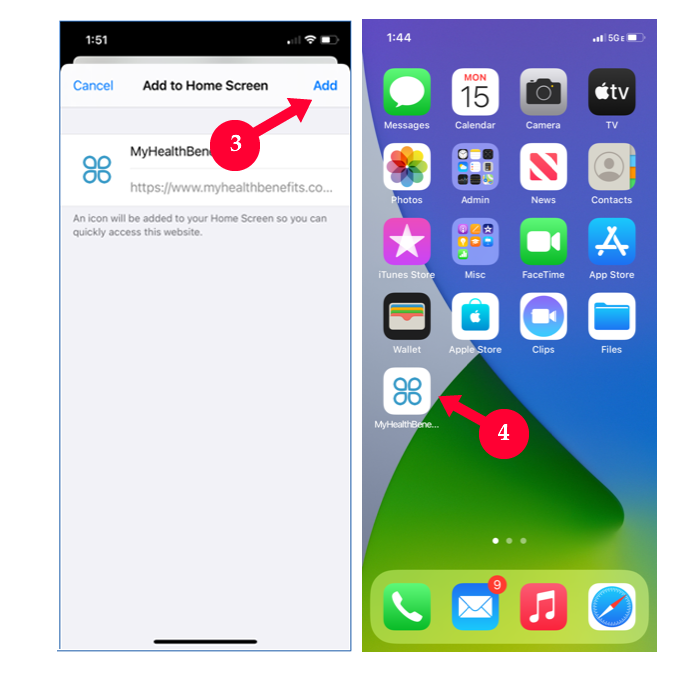
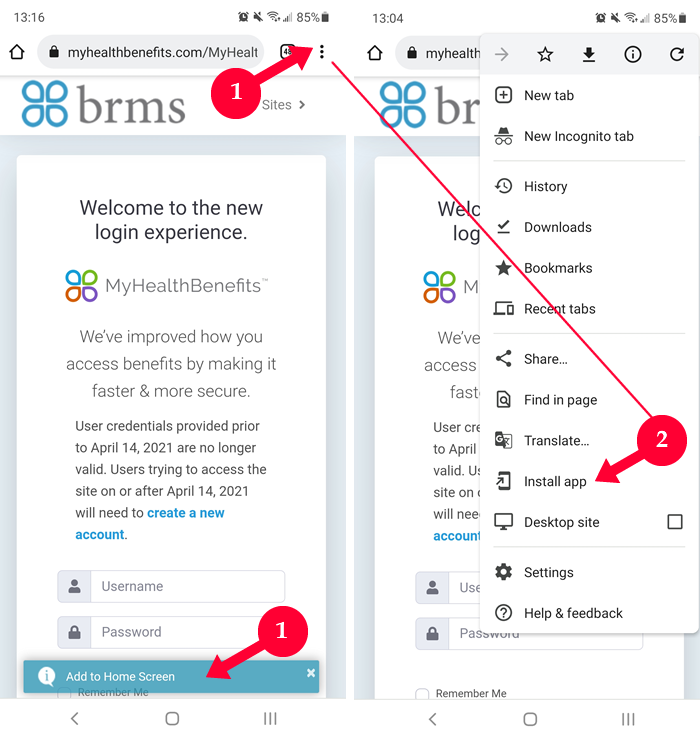
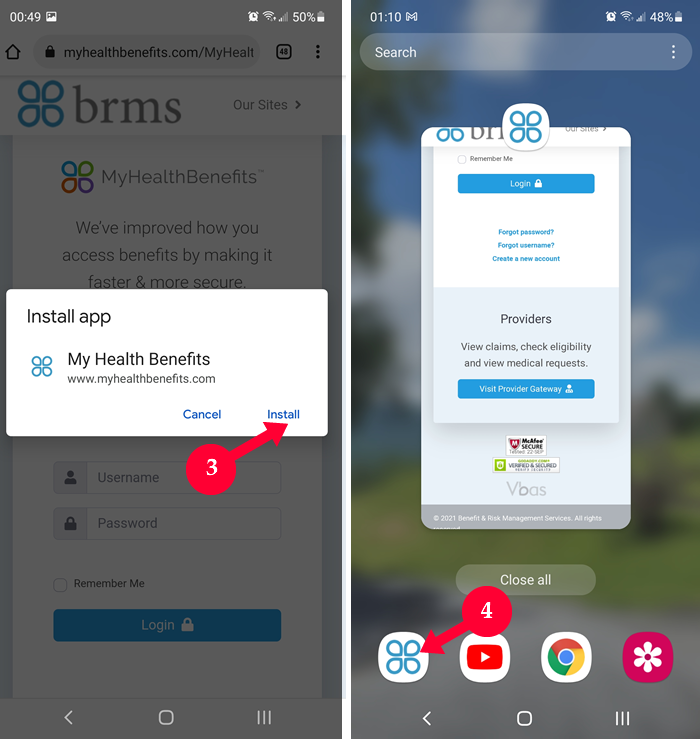
MyHealthBenefits Mobile
All features and capabilities of MHB are now mobile-friendly. To experience the mobile-friendly version of MHB, please click on the type of mobile device you have and follow the steps provided.